EYE CONDITIONS
Listed below are some of the eye conditions that our team at West Toronto Eyecare. To learn more, please click on the name of the condition.
Age-Related Macular Degeneration (AMD) is a chronic, age-related, degenerative disease of the macula. The macula is a very small and specialized area in the centre of the retina. The macula allows you to see fine details directly in front of you such as works in a book, images on television or details of a face.
There are two types of AMD, Dry AMD and Wet AMD. Generally, dry AMD progresses slowly and us usually less severe than the wet type. But both types damage the macula and both can take away your central vision.
Because AMD affects only your central vision, you won’t ever be totally blind. You will still have your peripheral, or side vision, and with the help of vision rehabilitation and vision aids, you should still be able to maintain your independence.
Risk Factors
- Age: Risk increases with advancing age; from 8.5% for people 43-54 years of age to a high of 36.8% for people over 75
- Family history of AMD
- Gender: Females are more susceptible
- Smoking
- Diet: A diet low in antioxidant vitamins and minerals
- Excessive sunlight exposure
- High blood pressure
- Excessive weight/obesity
What is dry AMD?
Most of the time, AMD will begin as the less severe dry type and, for 85-90% of people, it will remain that way. Dry AMD can develop in one eye or both.
The early stage of dry AMD usually begins with the appearance of yellow deposits called drusen. As the retinal layer continues to break down, an abnormal amount of drusen begins to build up. This build-up damages the layer of photoreceptor cells (the cells that receive visual images from the lens), resulting in blind spots in your central visual field.
As the disease continues to progress, the likelihood of it turning into the more severe wet AMD increases as well. According to the Age-related Eye Disease Study (AREDS), a large North American study of the effects of vitamins on dry AMD, up to 43% of people with late stage dry AMD can progress to the even more aggressive wet form of AMD within five years.
How is dry AMD diagnosed?
Dry AMD might first be noticed during a routine eye examination by your eye doctor, or because you noticed a change in your vision.
What is the treatment of dry AMD?
Treatment of dry AMD is focused on monitoring and slowing the progression of the disease. You should also consider making any modifications to your lifestyle that will help to slow the progression of the disease such as stopping smoking. Your eye doctor will discuss all of these options with you. You will be given an Amsler grid, that you should look at several times a week, one eye at a time, to help you determine if you are developing increasing blurred vision, new blank spots or distortion. Distortion of straight lines is an early sign of progression to wet AMD. The use of vitamin supplements may be discussed with you as well as dietary changes as these may diminish the rate of the progression of disease.
What is wet AMD?
Wet AMD is so named because of the involvement of blood in the deepest layers of the retina. In a process called choroidal neovascularization (CNV), new and abnormal blood vessels spontaneously begin to grow beneath the retina and push their way up through it. These new vessels leak their content of blood and fluid into the retina that disrupts the photoreceptors (the cells that receive visual images). This results in “blank” or blind spots in the central visual field.
Left alone, this process eventually results in the growth of scar tissue, which in turn, causes severe and permanent central vision loss. Perhaps surprisingly, there is no pain associated with the entire process. Although wet AMD can occur spontaneously, it’s usually preceded by dry AMD. Which makes regular check-ups especially important. Wet AMD is more aggressive than dry AMD and does not occur as frequently, accounting for approximately 10-15% of all AMD cases. It can cause rapid, sever and permanent central vision loss in a matter of weeks. Early detection is critical in order to start any treatments that might help preserve your vision.
What are the symptoms of wet AMD?
- Blurred vision
- Straight lines appear wavy or distorted (metamorphopsia)
- Blank spots in central vision (scotoma)
- Loss of colour perception
- Decrease in contrast sensitivity
How is wet AMD diagnosed?
Your regular eye doctor can usually diagnose wet AMD based on your symptoms, medical history and a dilated examination of your eye. After the diagnosis is made you will likely be referred to a retinal specialist for a definitive diagnosis and treatment. You will likely have an Optical coherence tomography test (OCT), a specialized test to look at a cross section of the retina and an intravenous Fluorescein Angiogram (IVFA) a series of photographs to visualize abnormal blood vessel leakage into the retina. Based on these tests possible treatments will be discussed.
What is the treatment of wet AMD?
There is no outright cure for age-related macular degeneration, but some treatments may delay its progression or even improve vision. For wet AMD, treatments aimed at stopping abnormal blood vessel growth include medications such as Lucentis, Avastin. Lucentis. has been shown to improve vision in a significant number of people with macular degeneration. The medication is given as injections into the eye until the wet macular degeneration is stabilized.
Nutrition and Macular Degeneration
Many researchers and eye care practitioners believe that certain nutrients; zinc, lutein, zeaxanthin and vitamins A, C and E help lower the risk for AMD or slow down the progression of dry macular degeneration. The Age-related Eye Disease Study (AREDS) published in 2001 was a major study sponsored by the National Eye Institute (NEI). In the study, scientists looked at the effects of zinc and antioxidants for halting or slowing development of macular degeneration. The study found that high levels of antioxidants and zinc can reduce the risk of vision loss from advanced AMD by about 19% in high-risk patients (patients with intermediate AMD or advanced AMD in one eye but not the other). Supplements do not provide significant benefit to patients with minimal AMD and do not seem to prevent the initial development of AMD, nor do they improve vision already lost to AMD. The long-term effects of taking large doses of these supplements are still unknown.
Phase two of the AREDS study began in late 2005 to evaluate whether similar protective effects against AMD might be associated with other nutrients such as omega 3 fatty acids or “good fats,” and lutein and zeaxanthin found in green, leafy vegetables.
Recent studies have found that consumption of omega-3 fatty acids, which are particularly prevalent in cold-water fish, also had a protective effect against advanced macular degeneration.
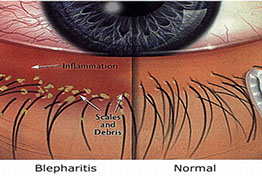 Blepharitis is a common eye condition that can occur at any stage in life. It tends to be chronic and recurrent. There may be a history of styes or recurrent “pink eye” in the past. In some cases it runs in families. In adult years it may be associated with acne rosacea, where pustules and dilated blood vessels appear on the face. The exact cause is unknown, but it is thought to be a disturbance of the oil production in the eyelid glands. Infection and tear film disturbances may occur secondarily. Contact lens wear can be quite difficult with any degree of blepharitis.
Blepharitis is a common eye condition that can occur at any stage in life. It tends to be chronic and recurrent. There may be a history of styes or recurrent “pink eye” in the past. In some cases it runs in families. In adult years it may be associated with acne rosacea, where pustules and dilated blood vessels appear on the face. The exact cause is unknown, but it is thought to be a disturbance of the oil production in the eyelid glands. Infection and tear film disturbances may occur secondarily. Contact lens wear can be quite difficult with any degree of blepharitis.
Symptoms Include:
- Burning, grittiness, foreign body sensation
- Redness, particularly along the lid margins
- Crusting along the lashes
- Blurring of vision
Management of Blepharitis
- Daily hygiene is an important part of maintaining a healthy ocular environment.
- Prepare your eyelids with a warm compress. Place a clean washcloth under hot tap water. Wring it out, fold it and hold it over both eyelids. After the cloth cools repeat the cycle for five minutes. The warm compress will help soften and loosen the residue and buildup on your eyelid. As well, it will increase blood circulation to the area to help combat the disease.
- Clean the margins or edges of your eyelids using the facecloth wrapped around your finger or with a recommended eyelid cleansing product.
- Use liberal amounts of artificial tears during the day.
- Minimize contact lens use or consider disposable lenses.
- Some cases require topical antibiotic and/or topical anti-inflammatory medications.
- Some cases require systemic antibiotic pills (such as tetracycline).
- The above treatments help to relieve the symptoms of blepharitis, however, the course of treatment is often long. Eventually you will learn to recognize the symptoms and treat yourself accordingly.
What are cataracts?
Much like a camera, the eye also has a lens within it. When this lens becomes cloudy, it is called a cataract.
Why do cataracts cause problems?
Cataracts prevent clear images from reaching the retina (the light-sensitive tissue at the back of the eye). In addition to causing blurry vision, cataracts may also produce glare, haloes, loss of contrast, and fading of colours.
When should cataracts be removed?
Cataract surgery is indicated when they cause enough problems that they interfere with your ability to enjoy or perform your daily tasks. These include driving, reading, sewing, and other daily activities.
What happens during cataract surgery?
You will be given a local anesthetic (i.e. The eye will be numbed with medications) and you will remain awake throughout the procedure. A small incision will be made and the cloudy lens will be removed with a special ultrasound, a procedure called phacoemulsification. After removal of the lens, a clear plastic lens called an intraocular implant (IOL) will be placed into the eye to replace the function of your natural lens that has been removed. Following the surgery, a shield will be placed over the eye before you are brought to the recovery area.
What needs to be done to prepare for cataract surgery?
Special measurements of your eye will be taken to determine the correct implant required for your eye. This will be arranged at the office and can be done with either laser or ultrasound. Eye drops will be prescribed for you to take three days before your surgery. They will help prepare the eye for surgery.
No food is to be taken after midnight the day of surgery. Clear fluids should not be taken 4 hours before your surgery. Regular medications (except diabetic medication) should be taken with a sip of fluid the morning of your surgery. Additional eye drops will be given once you arrive at the hospital.
What happens after cataract surgery?
After about an hour in the recovery area, patients are usually able to go directly home, with the assistance of a friend or family member. Most patients will experience some mild eye irritation or discomfort for the first one to two days following surgery, Regular or Extra-Strength Tylenol may be taken.
After your patch is removed, eye drops will be started and will be used for approximately 3-4 weeks after surgery. You will have a follow-up visit with your doctor, either the day of surgery or the day after surgery and the week after surgery. A new prescription for glasses will be given 4 weeks after surgery.
What activities are allowed after cataract surgery?
There are few limits on activities after surgery. You can read and watch TV almost right away, although your vision may still be somewhat blurry. Simple tasks such as climbing stairs or walking outside are allowed. Avoid eye rubbing or heavy strenuous activity for approximately 2 weeks. Avoid getting water in the eye and swimming for 1 week after surgery.
What are the benefits of cataract surgery?
Normal or near normal vision may be regained after cataract surgery, if the rest of the eye is healthy. In most cases, it takes the eye approximately 4 weeks to fully heal. Although many patients find much brighter vision and improved colour contrast soon after surgery, it may take several weeks for sharpest vision to return.
What are the risks of cataract surgery?
Cataract surgery is very successful with over 95% of patients having improved vision following surgery, However, as with any surgery, there are risks:
- Infection or bleeding in the eye. This is the most serious and rare risk (1 in 1500). This could lead to loss of vision in the eye.
- Retinal detachment (1 in 100)
- Glaucoma. This is usually temporary and can be treated with eye drops.
- Need for additional surgery. This occurs when not all of the cataract can be removed safely during the initial surgery (1 in 500)
- Swelling of the retina. This usually occurs weeks or months after surgery and can be treated with eye drops.
When should I call the doctor?
Call the doctor immediately if:
- You have a sudden loss of vision.
- The eye becomes very painful.
- There is a lot of discharge from your eye.
You should go to our Emergency Department outside regular office hours. Please ask your doctor if there are any further questions.
What drops do I use before and after cataract surgery?
Please refer to this sheet outlining information about medication you should take before and after surgery.
A chalazion is a lump along the eyelid margin. It occurs when the oil (meibomian) gland in your eyelid becomes blocked. It can be annoying but it is usually not painful and is rarely serious. Chalazia will often go away in a few months without treatment. Sometimes the swelling and inflammation can spread to the surrounding eyelid tissues.
Treatment for chalazia
- Warm compresses placed on the eyelid for 5 minutes twice a day may help to open and drain the clogged gland. Do not try to squeeze the chalazion.
- Antibiotic ointments may be prescribed if there is any associated infection with the chalazion
- Steroid injections or ointment may be used to reduce inflammation;
- Surgery may be used to drain a large chalazion if it does not respond to other treatments. This procedure can be done in the out-patient treatment room of the hospital.
What to expect with Chalazion Incision and Drainage:
The procedure only takes a few minutes. The eyelid is frozen using a small needle. Working from the inside of your eyelid your doctor will make a very small incision in the cyst and drain the contents. The eye is patched for one hour. You can continue with your normal activities for the rest of the day.
Chalazions usually respond well to treatment but some people are prone to recurrences. If a chalazion recurs in the same place, your ophthalmologist may suggest a biopsy to rule out problems that are more serious.
Diabetes is a condition in which the body does not properly regulate and use sugar (glucose) for its energy needs, usually because of failure to produce enough of the hormone known as insulin. Insulin is a hormone that controls the amount of glucose in the blood. The disease affects more than three million Canadians. There are two main types of diabetes that can affect the eyes. Type 1 diabetes, usually diagnosed in children and adolescents, occurs when the pancreas is unable to produce insulin. Approximately 10% of people with diabetes have type 1 diabetes. The remaining 90% have type 2 diabetes, which occurs when the pancreas does not produce enough insulin or when the body does not effectively use the insulin that is produced. Type 2 diabetes usually develops in adulthood.
How does diabetes affect the eyes?
Poorly regulated and high levels of sugar in the blood can cause changes in the optics of the eye, resulting in blurred vision and changes in eyeglass prescriptions. The condition may also interfere with focusing of the eye. Control of the blood sugar level usually corrects these problems. Diabetes can cause cataracts, double vision and glaucoma.
Diabetic retinopathy:
The most important cause of visual impairment in people with diabetes is diabetic retinopathy, a condition in which changes occur in the tiny blood vessels that nourish the retina (the light sensitive tissue that lines the back of the eye and changes the light into nerve message to be transmitted to the brain).
In the early stages of diabetic retinopathy, called non-proliferative or background retinopathy, small blood vessels weaken and leak fluid or tiny amounts of blood, which distort the retina. At this stage the person may have normal vision or may note blurred or changing vision. Although 25% of people with diabetes have some degree of non-proliferative retinopathy, the condition does not progress to more severe problems in most. In a more advanced stage, blood vessels in the retina are blocked or closed completely and areas of the retina die.
Proliferative diabetic retinopathy affects about 5% of people with diabetes and occurs when new, abnormal blood vessels grow to replace the old ones. These new vessels are fragile and often rupture and bleed into the eye, blocking vision. Scar tissue forms, shrinks and tears the retina, causing bleeding or detaching the retina from the back of the eye The growth of these vessels is triggered by a protein called vascular endothelial growth factor (VEGF). Anti-VEGF medicines block the effects of VEGF. Blocking this protein slows the growth of the abnormal blood vessels. Fortunately, proliferative diabetic retinopathy only occurs in a minority of diabetics.
The chance of having some form of diabetic retinopathy increase the longer a person has diabetes. Retinopathy is present in most people who have diabetes for more than 20 years.
How is diabetic retinopathy diagnosed?
Diabetic retinopathy is best diagnosed with a dilated eye exam. This allows your doctor to get a better view inside the eye. During the examination your doctor will look for:
- Abnormal blood vessels
- Swelling, blood or fatty deposits in the retina
- Growth of new blood vessels and scar tissue
- Bleeding in the clear, jelly-like substance (vitreous) that fills the centre of the eye
- Retinal detachment
Your doctor may request some additional testing such as fluorescein angiography and optical coherence tomography (OCT), to look for blood vessels that are closed or leaking. These tests can also be used to monitor progression of the disease and the effects of treatment.
What is the treatment for diabetic changes in the eye?
Proliferative diabetic retinopathy is treated with laser. This treatment is called pan retinal photocoagulation (PRP). In PRP your doctor places 1,000 to 2,000 laser burns in the areas of the retina away from the macula, causing the abnormal blood vessels to shrink. Because a high number of laser burns are necessary, two or more sessions usually are required to complete the treatment. Scatter laser treatment may slightly reduce your color vision and night vision. Injections into the eye of Anti-VEGF may be used in addition to the laser treatment.
Scatter laser treatment works best before the fragile new blood vessels have started to bleed. Even if bleeding has started, scatter laser treatment may still be possible, depending on the amount of bleeding.
If the bleeding is severe, you may need a surgical procedure called a vitrectomy. During a vitrectomy, a tiny incision is made in the eye. A small instrument is inserted into the cavity at the back of the eye and the gel containing the blood is removed. Vitrectomy is usually performed under local anaesthetic and you can usually return home on the same day.
Macular edema is treated with laser surgery or with injections of Anti-VEGF depending on the location of the retinal swelling. The laser procedure is called focal laser treatment. Your doctor places up to several hundred small laser burns in the areas of retinal leakage surrounding the macula. The burns reduce the amount of fluid in the retina. The treatment can be done in one session but you may require repeat treatments. Focal laser treatment stabilizes vision and reduces the risk of vision loss by 50%. Focal laser treatment can also be used to improve the effect of the Anti-VEGF injections in patients with macular edema.
If your doctor determines form angiography and OCT testing that injections are the best way to treat your eye, he/she with place the medicine into your eye using a very small needle. The injections takes just minutes and are usually well tolerated by the patient with only topical anaesthesia. Usually the treatment will start with 3 to 6 monthly Anti-VEGF injections. Additional injections will be determined your response to the initial injections. On average patients will receive 7 injections in the first year of treatment. Patients receiving Anti-VEGF injections may also have a laser treatment. Injections of steroids can also be of benefit in some patients who have diabetic macular edema and have had previous cataract surgery.
How do I develop dry eye?
Tears are produced by the lacrimal gland to protect the eye against infection and to comfort and lubricate the eye. Dry eyes are usually caused by reduced tear production or abnormal tear composition. Dry eye can be related to many causes including:
- Aging: people over age 50 and post – menopausal women are especially at risk for dry eyes
- Environmental conditions such as smog, smoke, dry environments and prolonged eye strain
- Diseases: asthma, blepharitis, Sjogren’s Syndrome
- Medications: antihistamines, decongestants, antibiotics, diuretics, blood pressure medications, chronic eye drop use
- Contact lens wear
What are the symptoms of dry eye?
Symptoms may include a burning or scratchy sensation. Some people feel as if they have sand or grit in the eyes. In more severe cases, some people may experience sensitivity to sunlight or blurred vision. There can even be uncontrolled tearing associated with dry eyes.
How are dry eyes treated?
Dry eye is usually a chronic problem with no cure. Simple measures such as remembering to blink frequently, avoiding smoky environments, using a humidifier in the winter and directing air vents away from the face can help reduce dryness.
Some patients find that eye drops can help with chronic dry eyes. There are many types of eye drops (ocular lubricants) on the market. Artificial tears used as needed, will usually provide relief from mild to moderate dry eye symptoms. In more severe cases lubricating gels or ointments, which have a longer lasting effect, may be used. Preservative free artificial tears may also be recommended for dry eye symptoms not controlled with other ocular lubricants.
Oral supplements containing omega 3 fatty acids such as flaxseed oil and fish oil may improve lacrimal gland function.
In severe cases, punctal plugs may be inserted into the tear drainage system to prevent tears from leaving the eye.
What are flashing lights?
Flashing lights are the sensation of lights, going on and off (similar to a lightning streak), noticed particularly off to one side. They tend to occur in only one eye at a time and persist even when the eye is closed.
What causes flashing lights?
The vitreous, a clear gel-like substance that fills the inside of the eye, can pull or tug on the retina. This pulling causes the appearance of flashing lights or lightning streaks, though there is no flashing light actually present. This same sensation sometimes occurs when on is hit in the eye and sees “stars”.
When the vitreous separates from the retina, flashing lights may appear periodically for a few weeks. This commonly happens as people grow older and usually is not cause for alarm.
Flashes of light that appear as jagged lines, last 10 to 20 minutes and are present in both eyes are more likely to be caused by migraine. If a headache follows it is called a migraine headache. If there is no subsequent headache, the light flashes are referred to as ophthalmic migraine.
Should you be concerned?
Most of the time the vitreous separates from the retina without causing any problems. Occasionally, flashing lights are associated with many new floaters and a shadow (like a blind or curtain) in part of the visual field. If this occurs, immediate examination by an ophthalmologist is important to determine whether a retinal tear or retinal detachment has developed. Retinal tears require treatment to prevent the retina from detaching. Retinal detachment is a serious problem that much be repaired with laser or surgery.
In summary, floaters and flashing lights usually do not indicate any serious eye problem. If a large number develop or they seem to be much worse of a period of time, an examination by an ophthalmologist is recommended. The examination involves careful observation of the retina and vitreous. Medical training and experience are required to perform this examination properly.
What are floaters?
Floaters are dark specks in the form of dots, circles, lines or cobwebs that appear to move across the field of vision. They are particularly noticeable when one is looking at a light-coloured background such as a clear sky or a white wall. Floaters come in may sizes and numbers, and they appear to move when the eye looks in different directions.
What causes floaters?
The inside of the eye is filled with a clear gel-like substance called the vitreous. The vitreous helps maintain the shape of the eye and allows light to pass through to the retina. The retina is a thin, light-sensitive tissue that covers the inside back portion of the eye and works like the film in a camera. Floaters are small clumps of gel that form in the vitreous. Although they appear to be in front of the eye, they are actually floating in the vitreous and are seen as shadows by the retina.
The appearance of floaters may cause concern, especially if they develop suddenly. However, they are usually of little importance. As people get older the vitreous shrinks and often separates from the retina. By the age of 50 years the vitreous has separated from the retina in about 50% of all people. As the vitreous detaches, it causes floaters. At first the floaters may be quite annoying, but the brain gradually learns to ignore them, and after several months they are hardly noticed.
Should you be concerned?
Most of the time the vitreous separates from the retina without causing any problems. In some people there are adhesions between the retina and the vitrous, and tears in the retina may occur as the vitreous detaches. This may cause a small amount of bleeding inside the eye, which may appear as a group of new floaters. Retinal tears should be repaired immediately. This can usually be done as an outpatient procedure, without the need for admission to hospital. A tear in the retina can develop into a retinal detachment, a serious problem that requires a major operation to repair. Certain people, such as nearsighted people and those who have had a cataract operation or suffered an injury to the eye, are more prone to retinal tears. Occasionally, floaters result from inflammation within the eye or from crystal-like deposits that form in the vitreous. Any sudden onset of many new floaters or flashes of light should be evaluated by an opthlamologist.
What can be done about floaters?
Floaters may sometimes interferes with clear vision, often when one is reading. If a floater appears directly in your line of vision, move your eye around; this will cause the vitreous to swirl around and will move the floater out of your way. Looking up and down rather than back and forth will cause different currents inside the eye and may be more effective in getting the floater out of the way.
What is glaucoma?
Glaucoma is the term applied to a group of eye diseases that gradually result in loss of vision by permanently damaging the optic nerve. Damage to the optic nerve is generally (but not always) caused by high pressure inside the eye. The high intraocular pressure (IOP) is transmitted to the optic nerve where it can gradually damage the nerve fibers. If the pressure is left untreated the nerve fibers eventually die causing loss in the peripheral vision. Over time, untreated pressure can result in complete loss of vision. Early detection and treatment is essential to prevent severe visual loss and blindness. Unfortunately, you can't feel the pressure that causes glaucoma. You need regular eye exams to check the pressure and the health of the optic nerve.
Glaucoma is the second most common cause of vision loss in seniors in Canada. More than 250,000 Canadians have chronic open-angle glaucoma, the most common form of the disease.
What are the different types of glaucoma?
There are many different types of glaucoma. Most, however, can be classified as either open angle glaucoma, which are usually slowly progressive or angle-closure (closed angle) glaucoma which can present abruptly or progress slowly.
Open-angle glaucoma
Primary open-angle glaucoma (POAG) is by far the most common type of glaucoma. In Canada it accounts for 90% of glaucoma cases. Its frequency increases with age, because over time the drainage mechanism of the eye may become less efficient. The pressure within the eye, therefore, builds up painlessly and without symptoms. Vision loss is not obvious until late in the disease when the central vision is permanently affected.
Normal tension glaucoma is a variant of primary chronic open-angle glaucoma. This type of glaucoma is thought to be due to decreased blood flow to the optic nerve. This condition is characterized by progressive optic-nerve damage and loss of peripheral vision (visual field) despite intraocular pressures in the normal range. This type of glaucoma can be diagnosed by repeated examinations by the eye doctor to detect nerve damage or visual field loss.
Secondary open-angle glaucoma is another type of open-angle glaucoma. It can result from conditions such as: eye trauma, ocular inflammation (iritis), cataracts, diabetes and steroid medications. The treatment for the secondary open-angle glaucomas vary, depending on the cause.
Pigmentary glaucoma is a type of secondary glaucoma that is can occur in younger individuals. It can be inherited. Due to a particular configuration of affected eyes, pigment from the iris is rubbed off and dispersed into the fluid within the eye. These pigment granules can block the drainage system of the eye. The blocked drainage system leads to elevated intraocular pressure, which results in damage to the optic nerve.
Pseudoexfoliative glaucoma is another type of secondary glaucoma. This type of glaucoma is characterized by deposits of flaky material on the front surface of the lens (anterior capsule) and in the drainage system of the eye. The accumulation of this material is believed to block the drainage system of the eye and raise the eye pressure. While this type of glaucoma can occur in any population, it is more prevalent in older people and people of Scandinavian descent. It is a systemic condition and recently has been associated with hearing loss in affected individuals.
Angle-closure glaucoma
In angle closure glaucoma the iris (the colored part of the eye) is pushed or pulled up against the drainage channel at the angle of the anterior chamber of the eye. When the iris is pushed or pulled up against the drainage system the fluid (aqueous humour) that normally flows out of the eye is blocked the pressure within the eye increases.
If the angle closes suddenly, symptoms are severe and dramatic. This is called Acute Angle Closure Glaucoma. Immediate treatment is essential to prevent damage to the optic nerve and vision loss. If the angle closes intermittently or gradually, angle-closure glaucoma may be have no symptoms until vision is severely affected.
People who are farsighted (hyperopic) are at an increased risk for acute angle-closure glaucoma because their anterior chambers are shallow and their angles are narrow.
Angle-closure glaucoma tends to affect people born with a narrow angle. People of Asian and Eskimo ancestry are at higher risk of developing it. Increasing age and family history are risk factors. It may be acutely triggered by medications that can dilate the pupils. This condition can also occur spontaneously in a darkened environment when the pupil automatically dilates to let in more light.
An attack of acute angle-closure glaucoma may be associated with headache, a severe red and painful eye, nausea and vomiting and blurred vision. In addition, the high intraocular pressure leads to corneal swelling, which causes the patient to see haloes around lights. Acute angle closure glaucoma is treated initially with topical and oral medications. The definitive treatment is usually laser surgery. In this procedure, the doctor makes a small hole in the iris with a laser (laser iridotomy) to re-open the drainage system and allow the fluid to resume draining into its normal outflow channels.
What are the risk factors for glaucoma?
- Family history of glaucoma
- Age
- Higher than normal intraocular pressure
- Suspicious optic nerve
- Thin corneas
- Myopia (nearsighted)
- African heritage
- Asian heritage (angle closure glaucoma)
- Use of medications such as steroids
- History of trauma to the eye
- Systemic vascular disease
What is the treatment of glaucoma?
The mainstay of glaucoma treatment is to lower the eye pressure, either with eye drops laser or surgery. A reasonable initial approach would be to choose an eye drop that will get the eye pressure as low as safely possible in each particular patient. The choice of the initial agent is guided by the patient characteristics and associated medical conditions and the known side effects of each medication. Each patient must then be monitored routinely to ensure that IOP is maintained at a level low enough to prevent glaucomatous progression. If additional eye pressure lowering is required then it is best to add an eye drop with a different mechanism of action than the initial drug.
If drops fail to maintain the pressure at the desired level laser (selective laser trabeculoplasty) can be performed. If both laser and medications are ineffective, the patient may undergo glaucoma surgery (trabeculotomy).
 A pterygium is an elevated, superficial, abnormal growth of
A pterygium is an elevated, superficial, abnormal growth of
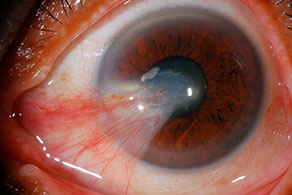
conjunctiva and fibrovascular tissue that invades the cornea. Pterygia can vary from small, quiet and slowly growing, to large, aggressive lesions that will grow to cover and distort the cornea.
What causes pteygia?
The main factor in their development seems to be increased ultraviolet exposure: including living in subtropical or tropical climates or engaging in occupations that require prolonged outdoor exposure. A genetic predisposition to the development of pterygia appears to exist in some families. Males have a prevalence of pterygia twice that of females. Dryness, ocular inflammation and exposure to wind and dust may also play a role in the development.
What are the symptoms?
Some patients with pteygia may not have any symptoms, while other may complain of significant redness, itching and irritation. Large pterygium can cause decreased vision by distorting the cornea (causing astigmatism) or scarring of the deeper layers of the cornea. Sometimes large pterygia can cause double vision when they involve the muscles of the eye.
How is pteygia treated?
It is advisable to wear ultraviolet blocking sunglasses to reduce the exposure to additional ultraviolet radiation. Patients with pterygia can be observed unless the lesion exhibits: growth toward the centre of the cornea, significant redness and irritation, or alterations in visual function. Medical therapy of pterygia is used for redness and irritation. It consists of topical lubricating drops and/or gels. A short course of topical corticosteroid anti-inflammatory drops may be prescribed by your doctor when symptoms are more severe.
Surgical Therapy
Pterygia can be removed because of severe irritation or visual disturbances. They may also be removed for cosmetic reasons. Surgery is usually performed as a day surgery under local anaesthetic with sedation if necessary. The pterygium is removed. The bare area is then covered with a small piece of conjunctiva removed from the same eye (conjunctival graft). Typically the graft is taken from an area under the upper eyelid and either glued or sewn in place. The eye is patched overnight. Topical antibiotic drops and topical anti-inflammatory drop will be used for up to two months following the surgery.
What is the prognosis?
The visual and cosmetic prognosis following excision of pterygia is good. The procedure is well tolerated. Some discomfort is expected for the first few postoperative days but patients can usually return to normal activities within a few days of surgery. Complications although uncommon include: recurrence of the pterygium, infection, reaction to suture material, corneal scarring, graft dehiscence and double vision. Recurrent pterygia can be treated with repeat excision and grafting.





